A Comprehensive, Evidence-Based Guide Eczema — also known as atopic dermatitis — is one of the most common chronic inflammatory skin conditions in the world, affecting an estimated 223 million people globally across all age groups. Characterized by dry, itchy, and inflamed skin, eczema can range from mildly irritating to severely debilitating, affecting sleep, mental …
A Comprehensive, Evidence-Based Guide
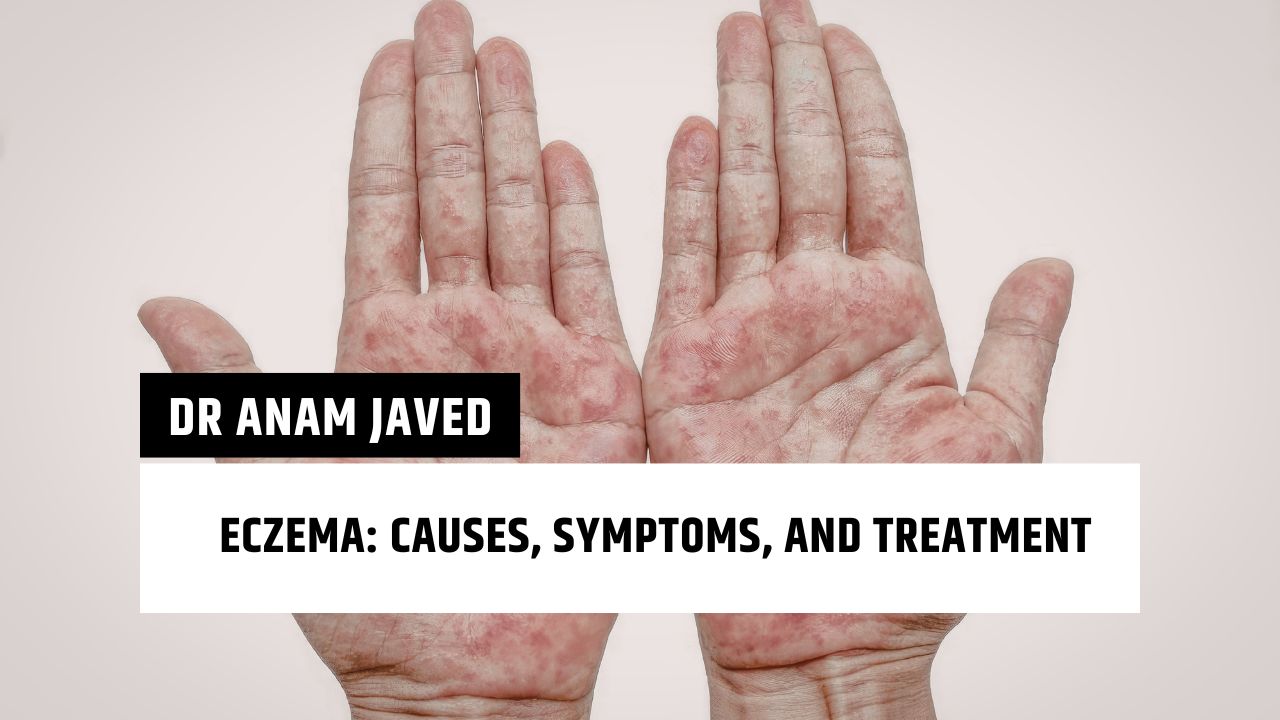
Eczema — also known as atopic dermatitis — is one of the most common chronic inflammatory skin conditions in the world, affecting an estimated 223 million people globally across all age groups. Characterized by dry, itchy, and inflamed skin, eczema can range from mildly irritating to severely debilitating, affecting sleep, mental health, and overall quality of life. Despite its prevalence, eczema is frequently misunderstood, misdiagnosed, or undertreated.
This comprehensive guide covers everything you need to know about eczema: what it is, why it develops, how to recognize its symptoms, the different types that exist, and the most up-to-date treatment options available. Whether you are newly diagnosed, caring for a child with eczema, or looking for better management strategies, this resource is designed to give you clear, reliable, and actionable information.
🔍 Key Fact: Eczema is not contagious. You cannot catch it from another person or spread it through skin-to-skin contact.
What Is Eczema?
Eczema is a chronic, non-contagious inflammatory skin disorder in which the skin barrier is impaired, making it unable to retain sufficient moisture and protect against environmental irritants, allergens, and microbes. The result is skin that is persistently dry, prone to itching, and susceptible to flare-ups — periods when symptoms intensify — often triggered by specific environmental, dietary, or emotional factors.
The word ‘eczema’ comes from the Greek word ekzein, meaning ‘to boil out,’ and historically referred to a broad category of skin inflammations. Today, the term is most commonly used to describe atopic dermatitis, though several distinct subtypes exist. ‘Atopic’ refers to the tendency for the body to produce exaggerated immune responses (atopy), and many individuals with eczema also have or develop related conditions such as asthma and allergic rhinitis — a triad known as the atopic march.
How Common Is Eczema?
Eczema affects people of all ethnicities, genders, and ages, but it is particularly prevalent in childhood. According to the National Eczema Association:
- Up to 25% of children worldwide are affected by eczema.
- Approximately 10–20% of infants develop eczema, with many improving or resolving by adulthood.
- Around 1 in 10 adults lives with some form of eczema.
- In South Asia, Southeast Asia, and parts of Africa, prevalence rates are rising alongside urbanization.
Eczema imposes a significant economic and psychological burden. Studies have shown that people with moderate-to-severe eczema report sleep disturbances, anxiety, depression, and reduced productivity at levels comparable to other chronic illnesses like diabetes and heart disease.
Types of Eczema
Eczema is not a single disease — it is an umbrella term for several related skin conditions that share features of inflammation, itching, and skin barrier dysfunction. Understanding the specific type you have is important for choosing the right treatment strategy.
1. Atopic Dermatitis (AD)
The most common form, atopic dermatitis typically begins in infancy or early childhood and is closely linked to genetic factors and immune system abnormalities. It is strongly associated with a family history of allergies, asthma, or hay fever. Atopic dermatitis tends to follow a relapsing-remitting course, with periods of flare and remission throughout a person’s life.
2. Contact Dermatitis
Contact dermatitis is triggered by direct skin contact with an irritant (irritant contact dermatitis) or allergen (allergic contact dermatitis). Common culprits include nickel in jewelry, latex, fragrances, preservatives in cosmetics, and cleaning chemicals. Unlike atopic dermatitis, contact dermatitis typically resolves once the triggering substance is identified and avoided.
3. Dyshidrotic Eczema (Pompholyx)
Dyshidrotic eczema causes small, intensely itchy blisters to form on the palms, fingers, and soles of the feet. Flares are often triggered by stress, sweating, seasonal changes, or contact with metals. This type disproportionately affects adults.
4. Nummular Eczema
Nummular (or discoid) eczema presents as round, coin-shaped patches of irritated skin, often on the arms, legs, or torso. The patches can be very itchy and may ooze. It is more common in men and older adults and may be linked to dry skin or prior skin injuries.
5. Seborrheic Dermatitis
Seborrheic dermatitis mainly affects areas rich in oil-producing (sebaceous) glands — the scalp, face (especially around the nose and eyebrows), and chest. In infants, it is commonly known as ‘cradle cap.’ In adults, it often takes the form of dandruff and may be associated with a yeast called Malassezia.
6. Stasis Dermatitis
Also called gravitational eczema, this type occurs in the lower legs of people with poor circulation, varicose veins, or swelling (edema). It is more common in older adults and can lead to open sores or ulcers if left untreated.
7. Neurodermatitis (Lichen Simplex Chronicus)
Neurodermatitis develops from repeated scratching or rubbing of a specific skin area. Over time, the skin becomes thick, leathery, and scaly. It often appears on the neck, wrists, forearms, or ankles and is associated with stress and anxiety.
What Causes Eczema?
Eczema does not have a single cause — it arises from a complex interplay of genetic, immunological, and environmental factors. Researchers continue to refine our understanding of eczema’s origins, but several key mechanisms are well established.
Genetic Factors
A strong family history is one of the most reliable predictors of eczema. Children born to parents with eczema, asthma, or allergies have a significantly elevated risk of developing the condition. One of the most important genetic discoveries in dermatology is the identification of mutations in the FLG gene, which provides instructions for making a protein called filaggrin.
Filaggrin plays a critical role in forming and maintaining the outermost layer of the skin — the stratum corneum. When filaggrin is deficient or absent, the skin barrier becomes ‘leaky,’ allowing moisture to escape and environmental allergens, irritants, and microbes to penetrate more easily. FLG mutations are found in approximately 30% of people with atopic dermatitis in Europe and North America.
Immune System Dysregulation
In eczema, the immune system is hyper-reactive. When the compromised skin barrier is exposed to environmental triggers, it initiates an exaggerated inflammatory response dominated by Th2 immune cells, which release cytokines — signaling proteins — such as interleukin-4 (IL-4), IL-5, and IL-13. These cytokines drive inflammation, itch, and further barrier disruption. This immune imbalance is the target of newer biologic medications used in moderate-to-severe eczema.
Environmental Triggers
Even in genetically predisposed individuals, eczema usually requires an environmental trigger to spark or worsen a flare. Common triggers include:
- Dry or cold weather that strips moisture from the skin.
- Heat and sweating, which can irritate sensitive skin.
- Harsh soaps, detergents, or shampoos containing fragrances or preservatives.
- Wool or synthetic fabrics that create friction.
- Dust mites, pet dander, mold, and pollen (aeroallergens).
- Food allergens (particularly in infants and children) — most commonly eggs, milk, peanuts, wheat, soy, and fish.
- Stress and anxiety, which can worsen inflammation and itch.
- Infections, particularly Staphylococcus aureus bacteria, which are found on the skin of most eczema patients.
The Microbiome Connection
Emerging research has highlighted the skin microbiome — the community of microorganisms living on the skin — as a major player in eczema. In healthy skin, diverse microbial communities help regulate immune responses and maintain the skin barrier. In eczema, the microbiome becomes less diverse and is often dominated by Staphylococcus aureus, which releases toxins that worsen inflammation and barrier dysfunction. Restoring microbial diversity is an active area of therapeutic research.
Signs and Symptoms of Eczema
The symptoms of eczema vary depending on the type, the severity, the patient’s age, and the stage of the disease. However, certain hallmark features are common across most forms of eczema.
Core Symptoms
- Intense itching (pruritus): Often described as the most distressing symptom, itching in eczema can be relentless. It tends to worsen at night, disrupting sleep and causing significant distress. Scratching provides only temporary relief and worsens the condition by further damaging the skin barrier — a cycle called the ‘itch-scratch cycle.’
- Dry, sensitive skin: The skin feels rough, tight, and parched even between flares. Moisturization is important even when symptoms are absent.
- Red or brownish-gray patches: In lighter skin tones, affected areas appear red or pink. In darker skin tones, eczema may appear as dark brown, purple, or ashen patches — a distinction that is important for accurate diagnosis.
- Small, raised bumps: In some presentations, tiny fluid-filled blisters may form that weep and crust over when scratched.
- Thickened, cracked, or scaly skin: Chronic scratching and rubbing cause the skin to thicken in a process called lichenification.
- Swollen or raw skin from scratching: Open skin increases the risk of bacterial, viral, and fungal infection.
How Symptoms Vary by Age
Infants (0–2 years)
Eczema in babies most commonly appears on the face, cheeks, scalp, and outer surfaces of the elbows and knees. The affected areas may look red and weepy. Babies often appear extremely uncomfortable, especially at night.
Children (2–12 years)
As children grow, eczema tends to migrate to the skin creases — the insides of the elbows, behind the knees, the neck, and around the wrists and ankles. The skin may become more dry and thickened than weepy. Many children see improvement during school-age years.
Adolescents and Adults
In teenagers and adults, eczema often persists in the flexural creases and may also affect the hands, feet, and face. Hand eczema is particularly burdensome for those in professions requiring frequent hand-washing. Adult-onset eczema can occur even without a childhood history.
⚠️ When to See a Doctor: Seek medical advice if your eczema is severe, infected (oozing yellow crust, increased redness, swelling), not responding to over-the-counter treatments, or significantly affecting your sleep and daily functioning.
How Is Eczema Diagnosed?
There is no specific blood test or imaging study for eczema. Diagnosis is clinical — meaning it is based on a careful examination of the skin, a review of medical and family history, and assessment of symptoms. Dermatologists use established criteria (such as the Hanifin and Rajka or UK Working Party criteria) to confirm an atopic dermatitis diagnosis.
Additional tests that may be ordered include:
- Patch testing: To identify specific contact allergens in cases of suspected contact dermatitis.
- Skin prick tests or specific IgE blood tests: To identify food or environmental allergens, particularly in children with severe or treatment-resistant eczema.
- Skin biopsy: Rarely needed, but may be used to rule out other skin conditions like psoriasis, fungal infections, or rare disorders.
Treatment Options for Eczema
There is currently no cure for eczema, but a wide range of treatments are available to control symptoms, prevent flares, and improve quality of life. Treatment is individualized based on the type and severity of eczema, the patient’s age, and response to prior therapies. A stepwise approach — starting with the most basic and least invasive measures — is typically recommended.
Step 1: Basic Skin Care — Moisturization
Consistent moisturization is the foundation of all eczema management. Applying emollients (moisturizers) frequently — ideally within three minutes of bathing — helps restore the skin barrier, reduce dryness, and decrease the frequency of flares. Dermatologists recommend:
- Thick creams or ointments (such as petroleum jelly or ceramide-containing creams) over thin lotions.
- Fragrance-free and preservative-free formulas to minimize irritation.
- Application at least twice daily, and more often in very dry conditions.
Wet wrap therapy — applying diluted topical corticosteroids under wet bandages — is sometimes used during acute flares to maximize absorption and reduce itch.
Step 2: Topical Corticosteroids (TCS)
Topical corticosteroids are the most widely used anti-inflammatory treatments for eczema. They are available in various strengths (potencies) and formulations, from mild hydrocortisone creams available over the counter to very potent prescription preparations. The correct potency and duration of use depend on the affected body area, patient age, and severity.
When used appropriately, topical corticosteroids are safe and effective. Overuse or misuse can lead to skin thinning, stretch marks, or systemic absorption in rare cases — risks that a dermatologist will help minimize through proper guidance.
Step 3: Topical Calcineurin Inhibitors (TCIs)
For sensitive areas such as the face, eyelids, and skin folds — where topical corticosteroids carry a higher risk of side effects — tacrolimus (Protopic) and pimecrolimus (Elidel) offer effective anti-inflammatory alternatives. These medications work by blocking the T-cell activation pathway. They are approved for use in patients over two years of age.
Step 4: Topical PDE4 Inhibitors
Crisaborole (Eucrisa) is a non-steroidal anti-inflammatory topical ointment approved for mild-to-moderate atopic dermatitis in patients as young as three months. It inhibits phosphodiesterase-4 (PDE4), reducing the production of inflammatory cytokines. It is a useful option when steroids and calcineurin inhibitors are not preferred.
Step 5: Systemic Therapies for Moderate-to-Severe Eczema
Biologics — Dupilumab (Dupixent)
Dupilumab is a monoclonal antibody that blocks the IL-4 and IL-13 signaling pathways — key drivers of atopic inflammation. Approved for patients aged six months and older, dupilumab has transformed the management of moderate-to-severe eczema. Clinical trials show significant reductions in itch scores, skin clearance, and quality-of-life measures. It is administered as a subcutaneous injection every two weeks.
JAK Inhibitors
Janus kinase (JAK) inhibitors, including abrocitinib (Cibinqo), baricitinib (Olumiant), and upadacitinib (Rinvoq), are oral medications that block intracellular signaling pathways involved in inflammation. They provide rapid relief of itch and skin inflammation and are approved for adolescents and adults with moderate-to-severe atopic dermatitis who have not responded adequately to other treatments. JAK inhibitors require monitoring due to potential effects on blood counts, lipid levels, and infection risk.
Traditional Immunosuppressants
Before the era of biologics, systemic agents like cyclosporine, methotrexate, azathioprine, and mycophenolate mofetil were used for severe eczema. They remain options in certain contexts, particularly when newer agents are not available or affordable, but require close monitoring for side effects.
Phototherapy (Light Therapy)
Narrow-band UVB phototherapy involves controlled exposure of the skin to specific ultraviolet wavelengths to reduce inflammation. It is an effective, medication-sparing treatment for moderate-to-severe eczema and is generally safe for adults and older children. Treatment typically requires visits two to three times per week for several weeks under medical supervision.
Antihistamines and Itch Relief
While antihistamines are commonly used for allergic conditions, the itch in atopic dermatitis is largely not histamine-driven, so traditional antihistamines have limited effectiveness in controlling eczema itch. Sedating antihistamines (such as diphenhydramine) may be used short-term to improve sleep during flares, but are not a primary anti-inflammatory treatment.
Treating Infections
Bacterial skin infections — most commonly caused by Staphylococcus aureus — are frequent in eczema patients and can significantly worsen flares. Treatment may include topical antibiotics (such as mupirocin) or oral antibiotics when infection is more widespread. Dilute bleach baths (using a small amount of household bleach in bathwater) have evidence for reducing S. aureus colonization and improving eczema severity.
Lifestyle Management and Prevention
Effective eczema management extends well beyond prescribed medications. Daily habits, environmental modifications, and awareness of personal triggers play a major role in reducing flare frequency and severity.
Identify and Avoid Triggers
Keeping a symptom diary can help identify personal triggers. Common ones to watch for include:
- Fabrics: Wear soft, breathable fabrics such as cotton. Avoid wool, synthetic blends, and tight-fitting clothing.
- Soaps and cleansers: Use gentle, pH-balanced, fragrance-free products. Avoid antibacterial soaps and bubble baths.
- Temperature extremes: Use a humidifier in dry environments. Dress in layers to avoid overheating.
- Stress management: Practice relaxation techniques such as mindfulness, yoga, or deep breathing. Psychological stress is a well-documented eczema trigger.
- Diet: In young children, supervised food elimination may be considered if food allergy is suspected. Adults are less likely to have food-triggered eczema, and dietary restriction should not be undertaken without medical guidance.
Bathing Practices
Bathing correctly is an important part of eczema self-care:
- Bathe or shower once daily in lukewarm (not hot) water for 10–15 minutes.
- Use a gentle, fragrance-free, soap-free cleanser.
- Pat — do not rub — skin dry with a soft towel.
- Apply moisturizer immediately after bathing while skin is still slightly damp.
Emotional and Psychological Support
The psychological impact of eczema is profound and often underestimated. Persistent itch, visible skin changes, and sleep deprivation contribute to anxiety, depression, and social withdrawal — particularly in children and adolescents. Seeking support from mental health professionals, eczema patient communities, and support groups (such as those run by the National Eczema Association) can be valuable parts of a holistic management plan.
Eczema in Children: Special Considerations
Managing eczema in infants and children requires special attention to safety, caregiver education, and age-appropriate treatments. The goal is not only to control symptoms but to protect a child’s development and wellbeing.
Early intervention is important. Studies suggest that applying emollients from birth in high-risk infants (those with a family history of atopy) may delay or reduce the development of eczema — though this area of research is still evolving. Parents should work closely with a pediatric dermatologist or allergist to develop a safe, effective, and sustainable management plan. Schools and childcare providers should also be informed to support the child’s comfort and minimize exposure to known triggers.
The Future of Eczema Treatment
Eczema research is moving at an exciting pace. Multiple new biologic agents targeting different inflammatory pathways — including IL-31, IL-33, IL-13, and thymic stromal lymphopoietin (TSLP) — are in advanced clinical trials. Tralokinumab (Adbry) and lebrikizumab (Ebglyss), both targeting IL-13, have already received regulatory approval in several countries, offering additional options for patients who do not respond to or tolerate dupilumab.
Microbiome-based therapies, including topical preparations containing live commensal bacteria, are also being investigated. Gene-editing approaches targeting FLG mutations represent longer-term possibilities. The rapid expansion of the treatment landscape means that more people with eczema — including those with the most severe and treatment-resistant disease — will have effective options in the years to come.
Conclusion
Eczema is a chronic, complex, and deeply personal condition that affects hundreds of millions of people worldwide. While it has no cure, it is highly manageable with the right combination of daily skin care, medical treatment, trigger avoidance, and psychological support. The treatment landscape has been dramatically transformed in recent years with the approval of targeted biologics and JAK inhibitors, offering hope for even the most severe cases.
If you or someone you care for is living with eczema, do not accept unnecessary suffering. Work with a qualified dermatologist or allergist to build an individualized management plan. With the right approach, most people with eczema can achieve significant symptom control and enjoy a high quality of life.
📌 Always consult a board-certified dermatologist or healthcare provider for a personalized diagnosis and treatment plan. The information in this article is for educational purposes and does not substitute for professional medical advice.
SEO Metadata
Focus Keyword: eczema causes symptoms and treatment
Meta Description (150 chars): Learn about eczema causes, symptoms, and proven treatments. Expert guide covering types, triggers, medications & skincare for all ages.
Keywords: eczema, atopic dermatitis, eczema causes, eczema symptoms, eczema treatment, skin inflammation, eczema in children, eczema remedies, topical corticosteroids, dupilumab, eczema triggers, dry skin, itch relief, contact dermatitis, skin barrier, eczema flare, biologic for eczema, JAK inhibitors, nummular eczema, dyshidrotic eczema